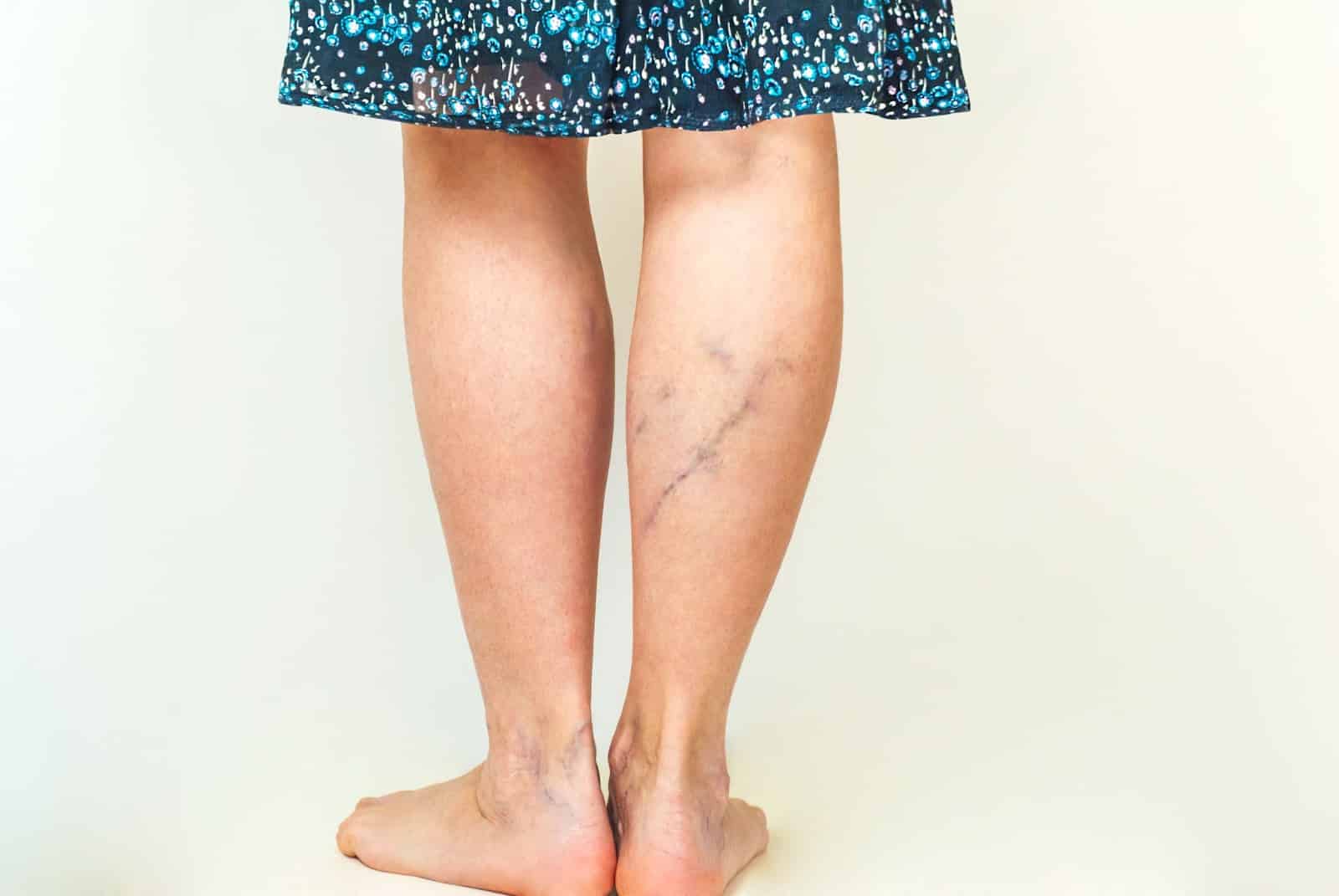
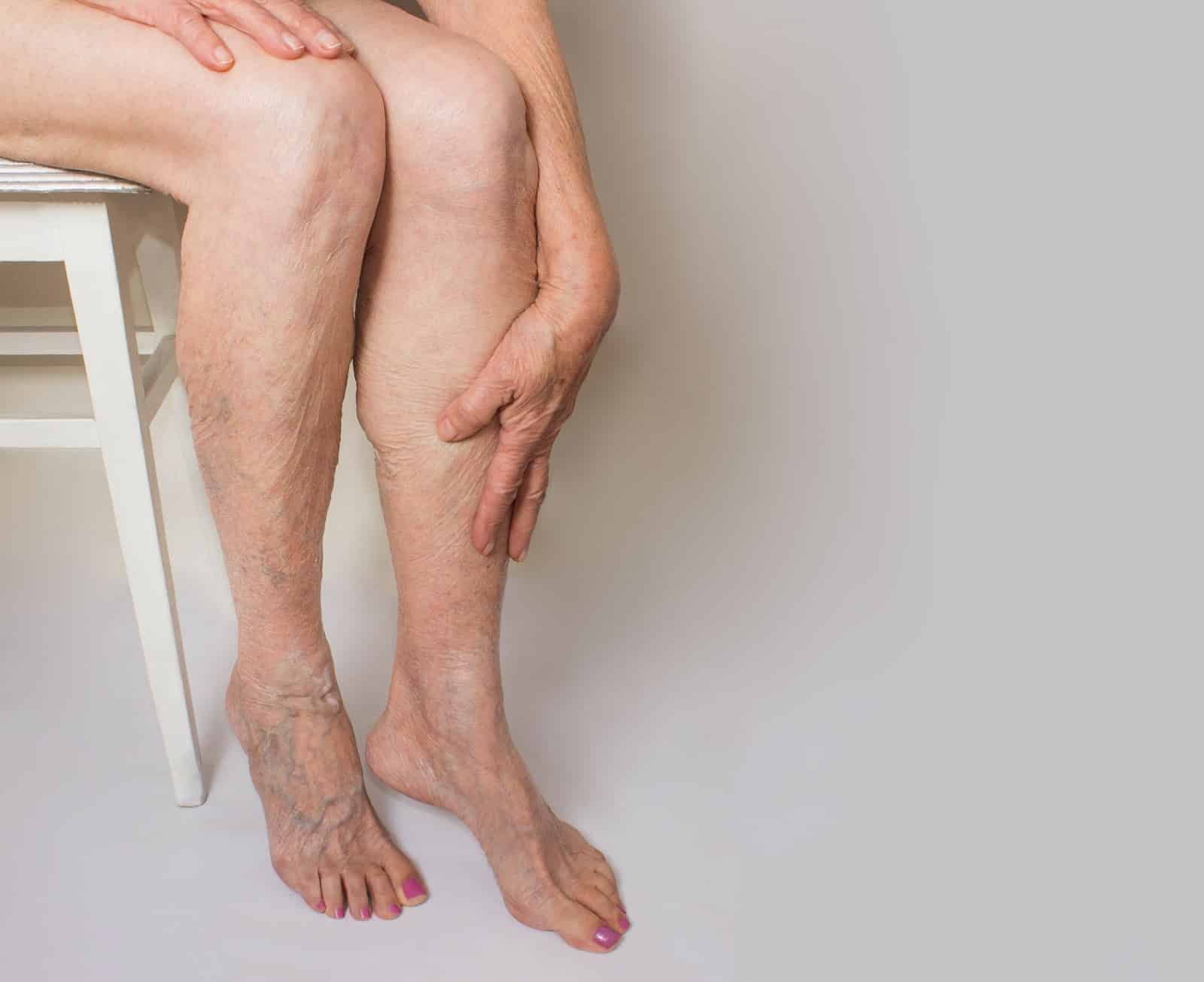
Varicose veins are a chronic venous disease affecting millions of women and men in the US. Nearly one in four US adults will develop varicose veins during their lifetime. Women in the age group of 40 to 80 are a high risk group for chronic venous insufficiency, varicose veins and spider telangiectasias.
When varicose veins are relatively minor or have newly appeared, they may be painless and are widely perceived as a cosmetic issue. Taking this into account, varicose veins may indicate serious underlying conditions. If left untreated, they can lead to serious venous complications and reduce an individual’s quality of life.
What are Varicose Veins?
Varicose is the medical term for dilated veins that are more than 3mm in diameter. The diameter of spider veins is smaller, less than 1 mm. Reticular veins are those with a diameter of more than 1 mm but less than 3 mm.
Many people make the mistake of ignoring them as purely a cosmetic issue, but over time varicose can pose significant health risks. Sometimes, they may indicate a blood clot or a deep vein thrombosis. If not treated quickly, conditions such as deep vein thrombosis can turn out to be fatal. Other risks associated with varicose veins include skin allergies, venous ulcers, and spontaneous bleeding.
Sclerotherapy treatment is one of the safest and most effective ways to get rid of minor varicose veins and spider veins. Laser vein treatments and microphlebectomy may also be used for more prominent varicose veins. Treated veins in the laser or injection site will gradually coalesce, turn into scar tissue, and get absorbed within the body.
What Causes Varicose Veins?
It’s an area of active research. Researchers continue to study what causes the blood circulation in a specific zone of your body to produce varicose veins. One of the more probable explanations is that some of the veins (especially in the legs) may have to deal with an increased blood flow all of a sudden. This hyperactivity exacerbates the condition when the valves in the veins are not working as they should.
Problems with Blood Flow
Normally, the blood flow in healthy veins represents a one-way passage. In accumulation of this, if the valves at vein junctions start to weaken, the blood may backflow and accumulate within the veins. Over time, the blood stress causes the walls of the veins to bulge, leading to the appearance of varicose and spider veins. When this condition affects a larger and more prominent vein in the legs, it’s called varicose.
Spider veins are similar to the larger varicose veins but they are smaller and more branched in appearance. The smaller veins may appear with or without large varicose veins.
Faulty Lifestyle Habits
Several factors may contribute to the formation of a varicose vein. Jobs that require a person to remain in a standing posture for extended time periods can lead to stress on the leg and feet muscles.
Obesity is also thought to be a contributing factor, and so are smoking and alcohol consumption. Junk food obsession, smoking, and alcohol consumption may cause the walls of the veins to thicken, leading to the formation of small varicose veins. Research suggests that genetics may also have a role to play in the formation of varicose veins.
Pregnancy Stress
Sometimes, expecting mothers may notice the formation of varicose veins on their lower legs and feet. The body of a pregnant woman undergoes a series of significant changes, and the appearance of varicose veins is sometimes a part of these changes. The growing weight of the body, constant hormonal changes, and increased blood flow during pregnancy may contribute to this condition.
During pregnancy, you should keep a close watch on the areas surrounding the veins. Consult the doctor if the veins start to ache or rashes appear. Moreover, varicose vein treatments, such as sclerotherapy, should be put on hold while you are pregnant or breastfeeding.
Health Risks Associated with Varicose Veins
Assuming that varicose veins are merely an aesthetic concern and ignoring treatment for varicose veins can pose risks to your health and well-being. Sometimes larger varicose veins can become so taut and sensitive that they may start to bleed with the slightest stimulus. Even the simplest act of drying yourself with a towel can break the skin over the varicose veins. Initially, the skin turns brown or red. It also becomes hot or painful in the regions near the affected veins. It can lead to more serious venous complications over time.
Symptoms to Watch Out for
When should you seek vein treatment? Women often seek sclerotherapy treatments merely because the gnarly varicose veins do not look good on the legs. In relation to this, it would be a mistake to understand the conspicuous leg veins merely as a cosmetic issue. While aesthetic appeal is important for your self-image and self-confidence, you should also focus on the potential symptoms that indicate a serious underlying health concern. Common symptoms include:
- Dullness in the legs
- Constant aching in the affected areas
- Sleep disruption
- Throbbing sensation
- Swelling and inflammation
- Skin rash around the varicose veins
- Feeling heaviness in the legs
If one or more of these symptoms persist, you should contact a vascular specialist. The doctor will conduct a series of blood tests or an ultrasound exam, and evaluate the abnormal leg veins to determine if they pose a risk to your health.
Sclerotherapy of varicose veins is a quick and painless procedure. It can be done on an outpatient basis, without the requirement of incision or anesthesia. Similarly, laser vein treatment is another highly effective in-office procedure to eliminate varicose veins and spider veins. Your doctor may also suggest that you wear compression stockings for a certain period of time to help restore normal blood flow in veins.
Not Just a Grandma’s Disease
You might be familiar with varicose veins if you saw them in the back of your grandparent’s palms. Such veins are quite commonly seen in older adults. Aging causes the valves of veins to weaken, and as a result, the blood in the vein becomes sluggish and accumulates. But it’s fundamental to understand varicose veins do not affect only the elderly. They can cause pain, discomfort and health complications at any age.
Initially, the veins may seem just like an unsightly cosmetic issue. You might think that they are harmless, and may require some treatment only years or decades from now. Stemming from this, in reality, varicose veins is not just a grandma’s disease. Many people in younger age groups may suffer from complications and a poor quality of life because of chronic venous insufficiency.
Different treatment plans are available including laser therapy for varicose veins. Sclerotherapy for varicose veins is one of the popular procedures. One in-office treatment session does not last more than an hour and you can return to normal activities very soon.
Following the treatment session, you may need to wear support hosiery to maintain a uniform pressure on the veins treated. Walking is a recommended activity to maintain normal blood flow in the veins. Also, as long as the treated veins do not disappear completely, you should avoid a hot bath, sauna, or prolonged sun exposure. The doctor will recommend against using blood thinners and antibiotic medications during the post-treatment recovery period.
Veins Have to Resist Gravitational Forces (Fight Against Gravity)
Leg veins are more prone to become varicose because the blood must fight against the gravitational pull. The network of veins carries blood from all parts of the leg toward the heart. Veins connect via a series of one-way valves. these valves open up with upward pressure to let blood flow toward the heart. They again close back to prevent backflow, until the next blood flow arrives.
Other veins in the leg connect to form the saphenous vein. This is the key vessel to carry deoxygenated blood to the heart. Each leg has two saphenous veins. These are the great saphenous vein and the small saphenous vein.
Furthermore, the valves in the veins leading to the saphenous vein may become weak or damaged with time. This results in a backflow of the blood. As a result, the veins become enlarged and are visible through the skin. Venous insufficiency refers to this condition of blood pooling inside the veins. Insufficiency causes the vein walls to stretch. The stretching creates a domino effect affecting a network of subsequent veins. This action results in the formation of spider veins.
Sclerotherapy and cutaneous laser therapy can successfully treat varicose veins. These treatments can usually result in the complete disappearance of the diseased veins within three to six weeks. Timely treatment can prevent further complications of varicose veins.
Potential Complications When Varicose Veins are Left Untreated
Awareness about the potential health complications of varicose veins can help you prevent a medical emergency later on. You should keep a close watch on mild aching, dullness, and other related symptoms in the legs when varicose veins are present. In most cases, varicose veins respond quite well to sclerotherapy or laser vein therapy.
The vein specialist will assess your medical history to determine whether you are an eligible candidate. Several factors are taken into account including the medications you are on, whether you have had a vein treatment before, and if you are comfortable with a fine needle or laser treatment. Patients who have a medical history of forming frequent blood clots should not undertake varicose vein treatments.
Ignoring or delaying varicose vein treatment for a long time may lead to one or more of the following health complications in some cases.
Superficial Thrombophlebitis
Superficial thrombophlebitis indicates a vein blockage scenario near the surface of the skin. Reasons may include trauma, prolonged periods of inactivity, or a surgical error. The leg is the most commonly affected region and the vein becomes swollen, reddish, and tender to touch. Apart from the swelling, the condition is accompanied by deep pain in the affected veins.
The blockage is caused due to formation of a blood clot inside the vein. As the vein becomes varicose, it increases the risk of pulmonary embolism. If the blood clot breaks away and travels to the lungs, it may lead to chest pain that ultimately turns fatal. Such a situation demands immediate emergency medical attention.
Varicose veins may lead to the development of superficial thrombophlebitis. Apart from the risk of forming pulmonary embolism, the condition may worsen into a swelling of the leg. The swelling and leg pain is also known as post-phlebetic syndrome. The medical term for blood clotting in a deep-placed vein is deep vein thrombosis or DVT. Post-phlebetic syndrome can develop months or years after you had DVT. The pain is usually quite severe.
Have your varicose and spider veins treated with sclerotherapy, laser vein treatment or microphlebectomy. Timely treatment can minimize your risks of future complications.
Spontaneous Bleeding
Spontaneous bleeding can occur when the skin over the spider veins weakens over time. As the skin becomes vulnerable, the slightest pressure can rupture it and result in bleeding. Venous reflux or backflow of blood in a vein can create pressure over the skin over time, causing it to rupture.
Being obese or having a sedentary lifestyle can also increase the risk of spontaneous rupture. Over-exercising and relying on hormone injections to grow muscle mass can also increase the pressure on veins, making them varicose.
Intradermal bleeding refers to the situation when a spider vein ruptures beneath the skin’s surface. A skin injury can be a potential reason for causing intradermal bleeding. This bleeding is visible as a blue-purple bruise through the skin. Varicose and spider veins are also at an increased risk of cuts and nicks during leg shaving or any other external trigger.
Timely sclerotherapy of varicose veins can prevent the occurrence of these situations. Other options to treat varicose veins include microphlebectomy, cutaneous laser therapy, and foam sclerotherapy. In laser therapy, the trained specialist inserts a catheter into the affected vein through a very fine incision. After this, a laser fiber is put in the catheter. The application of laser energy causes the vein to dry up and close off eventually.
Sclerotherapy involves injecting a sclerosing agent into the vein in question using a very fine needle. The liquid or foam solution eventually achieves the same final effect as the laser therapy. The dried-up vein turns into scar tissue and gradually disappears into the body, leaving no visible trace.
Fatal Hemorrhage
Fatal hemorrhage is a rare medical condition when the spontaneous rupture of varicose veins results in the loss of life. Patients who have had previous instances of spontaneous bleeding are at an increased risk of fatal hemorrhage in the future. In addition, persons with coagulation anomalies should have their veins checked with a specialist to prevent the chances of such an occurrence.
Sclerotherapy and laser vein treatment are relatively simple and minimally invasive medical procedures, which can mitigate or entirely eliminate your risk of serious venous complications. You should check with your insurance provider if sclerotherapy or laser vein treatment at your doctor’s office is covered within your health plan.
Statis Dermatitis
Neglecting varicose and spider veins makes you vulnerable to developing a complex skin condition called statis dermatitis. The accumulation of blood due to venous reflux in the lower leg may eventually cause the capillaries at the feet to burst open. Along with blood, water also accumulates in the lower extremities. Symptoms include ankle swelling, skin discoloration, scaling, and dryness.
In extreme cases, varicose eczema may escalate to form venous ulcers. These ulcers become prone to bleeding, oozing, and they tend to leave unsightly scars on the feet. The smaller varicose veins are particularly vulnerable to growing into statis dermatitis. Timely sclerotherapy treatment or laser vein treatment can effectively prevent this occurrence in most cases. Allergic reaction to the sclerosing agent or laser heat reactions are extremely uncommon. In rare cases, patients may develop localized rashes or redness in the treated site, which will resolve soon.
Venous Statis Ulcers
Venous ulcers or leg sores can be very painful. If untreated, they can lead to necropsy and foot amputation. Preventive steps include quitting smoking, taking prescribed blood thinners, and maintaining a healthy weight. Based on this, if you are suffering from chronic venous insufficiency, the best preventive step is the early removal of varicose veins from the affected areas, such as legs, feet and ankles.
Lipodermatosclerosis
Prolonged negligence of varicose veins in the lower legs can lead to a severe skin condition called lipodermatosclerosis. The symptoms of this chronic inflammatory condition include heavy hardening of the skin. Venous insufficiency is the primary reason behind this condition. The backflow of blood in diseased veins of the lower leg results in an increase of white blood cells in that area.
These leukocytes spread to the surrounding tissue and become activated. These activated white blood cells further release proinflammatory cells and cytokines, which in turn, hypes up collagen production. The chain reaction continues and the collagen thickens to produce fibrosis of the subcutaneous fat and a dark skin tone. It’s a preventive condition, only when you don’t neglect the signs of early onset, and have your spider veins treated.
Deep Vein Thrombosis
Generally speaking, spider veins are painless and may not involve a serious health risk except aesthetic concerns. Taking this into account, larger veins may pose a serious risk of becoming varicose. One of the rare complications of untreated varicose veins is deep vein thrombosis. Blood clots in veins may indicate this condition. The underlying cause of DVT is excessive blood pooling in the affected areas where the vein function is abnormal.
Post-phlebitic syndrome and hemorrhages are potential complications that can develop with DVT. Symptoms of post-phlebetic syndrome include skin discoloration, skin sores, leg swelling, and pain. Doctors often administer blood thinners to relieve DVT. However, the thinners themselves increase the complications of internal hemorrhage. The doctor will regularly conduct blood tests while you are on blood thinners.
Pulmonary Embolism
DVT is more dangerous than superficial vein thrombosis and entails a greater health risk. This is because a blood clot may break and travel to the lungs, causing pulmonary embolism. The clot obstructs blood flow to the lungs. It’s a potentially life-threatening health condition, which is typically accompanied by acute chest pain and coughing.
Patients with previous underlying heart and lung diseases are at greater risk of pulmonary embolism. Common symptoms of pulmonary embolism include fever, excessive sweating, dizziness, and irregular heartbeat. This condition is a health emergency requiring immediate professional medical attention.
One of the ways to prevent or minimize the occurrence of DVT and subsequent pulmonary embolism is to get the varicose veins treated well in time. You need to visit a specialist clinic to evaluate the possible treatment options.
Sclerotherapy, microphlebectomy, and laser treatment can effectively remove varicose veins. Microphlebectomy involves the administration of local anesthesia. After identifying the varicose veins, the doctor will remove them from the body through tiny sutures. Sclerotherapy and laser vein therapy are minimally invasive treatments for varicose veins.
Choose Mark Medical Care for Reliable and Advanced Treatments for Varicose Veins
Mark Medical Care is a highly rated medical office for the treatment of venous diseases. Led by experienced vein specialist Dr. Ron Mark, Mark Medical Care has been successfully treating patients with varicose veins and spider veins for more than a decade. The dedicated team of doctors at the facility speaks English and Spanish, which makes it easier for patients to communicate with their medical provider in their native language.
The state-of-the-art medical facilities at Mark Medical Care are equipped to perform advanced venous procedures such as sclerotherapy, laser vein treatment, and microphlebectomy. The office has received JCAHO accreditation. To book your appointment, give us a call at 877-673-4818 or contact us online.